LEPTO DIPSTICK: A LEPTOSPIRA SPECIFIC IgM ASSAY FOR USE ON HUMAN SERUM SAMPLES
INTRODUCTION
The human Lepto dipstick assay is a simple assay for the detection of Leptospira-specific IgM antibodies in human serum samples. The assay is rapid and requires no special equipment. The ingredients are highly stable and can be stored at room temperature (20°C-25°C). When tested on a group of sera from leptospirosis patients and negative control from the Netherlands the sensitivity and the specificity of the assay were found to be similar to those of ELISA for the detection of Leptospira-specific IgM antibodies.
PRINCIPLE
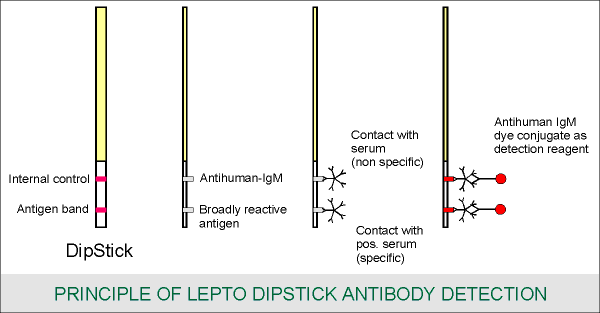
The dipstick contains two horizontal bands: an antigen band consisting of broadly reactive Leptospira antigen (lower band) and an internal control (upper band). The assay is based on the binding of human Leptospira-specific IgM antibodies to the Leptospira antigen. Bound IgM antibodies are specifically detected with an anti-human IgM dye conjugate. The broadly reactive Leptospira antigen ensures the efficient detection of a wide spectrum of Leptospira infections. The assay is performed by making a 1:50 dilution of serum in the detection reagent and incubating a wetted dipstick in this solution. Staining of the antigen band reveals the presence of Leptospira-specific IgM antibodies in the serum sample. The strength of the staining is important in the interpretation of the test results. The provided, colored reference strip is used to compare the staining intensity. The internal control band provides a check on the integrity of the detection reagent and the presence of serum.

REAGENTS
WARNING: THE RECONSTITUTION FLUID AND THE DIPSTICK FLUID CONTAIN SODIUM AZIDE. DO NOT SWALLOW AND AVOID SKIN CONTACT
UTENSILS (PROVIDED)
UTENSILS (NOT PROVIDED)
PACKAGE SIZE
Each package contains 20 dipstick and 3 reagents sufficient for the analysis of 20 sera.
STORAGE
Dipstick and reagents should be stored at +4°C to 25°C, in a dry place and protected from exposure to sunlight. Exposure to temperature up to 37°C for short periods (1 months) is allowable but not recommended. Storage at +4°C to 25°C is recommended for the reconstituted detection reagent. When stored at this temperature range the reconstituted reagent retains full reactivity for 1 month.
EXPIRY DATE
The ingredients expire on the date printed on the box.
PRECAUTIONS
Blood and serum samples should be handled carefully as they are potentially infectious. Equipment and supplies for specimen handing should be treated accordingly. Serum samples which have been heat-inactivated (56°C for 30 minutes) may be used, ass heat treatment does not affect the results of the assay. Used disposables and samples should be properly discarded.
SPECIMEN COLLECTION
Serum should be collected in the same way is routinely performed for any clinical laboratory assay.
STANDARD ASSAY PROCEDURE
Notes: Do not touch or bend the white test strip.
Contamination of the white test strip with traces of serum or blood at this point
may produce false positive results.
Contamination may occur due to handling and/or opening of serum ampoule, and
handling of liquids containing diluted serum.
Notes: Placing a dry dipstick into the mixture of reconstituted detection reagent and serum without previous wetting of the white test strip will result in a high background staining. Incubation of the dipstick for more than 1 minute may result in loss of activity.
Notes: The above procedure is designed and optimized for performance at 18°C to 25°C. Equal results have been obtained when performing the assay at 37°C with a reduced incubation period (step 6) of 2 hours.
INTERPRETATION OF ASSAY RESULTS
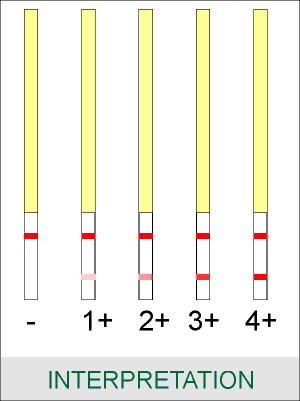
Use the colored reference strip to determine the staining intensity. Staining of the antigen band (lower band) reveals the presence of Leptospira-specific IgM antibodies in the serum sample. A straining intensity rated 2+ or more provides evidence for current or recent leptospirosis. If staining is weak (1+) or not present, and suspicion of leptospirosis remains the assay should be performed on a second sample taken at a later date in conjunction with a re-examination of the first sample to look for an increase in the amount of antibodies or seroconversion. An increase in the amount of antibodies will result in a intensification of the staining of the antigen band. The internal control (upper band) should stain in all cases. If the internal control does not stain the assay is invalid. The staining intensity of the internal control band may vary from patient to patient but will be 2+ to 3+ in most cases.
Note: The colors of the developed dipsticks and the colored reference strip may fade when exposed to light. Developed dipstick and the reference strip should be stored in the dark.
LIMITATIONS OF USE
As with any diagnostic test, results from the Lepto dipstick should be interpreted with consideration of the clinical, epidemiological and other laboratory findings.
Antibodies usually become detectable 7-10 days after the onset of the disease and sometimes even later. Early antibiotic treatment may suppress antibody production.
Although the results of the Lepto dipstick are found to be in agreement with those of the ELISA for the detection of Leptospira-specific IgM antibodies neither 100% sensitivity nor 100% specificity is claimed.
False-positive reactions may occasionally occur with sera from patients with diseases other than leptospirosis. However, only a low staining intensity has been observed in such cases.
False-negative reactions occasionally may occur when either only serovar specific antibodies or when IgG antibodies rather than IgM antibodies are formed.
Confirmation with MAT is recommended.
ADVANTAGES OF THE LEPTO DIPSTICK
REFERENCES
![]()